Share this article:
Written by: Dr. Glenn

What is Sciatica Pain & Its Symptoms
Sciatica is not a standalone condition; it can be better explained as a symptom indicating an underlying issue, often related to the compression or irritation of the sciatic nerve. The sciatic nerve, the longest nerve in the human body, extends from the lower back, traversing through the buttocks and down each leg. Pain associated with sciatica primarily occurs along this nerve pathway. Individuals grappling with sciatic pain may experience a range of sensations, including sharp shooting pain, numbness, tingling, and weakness.
Triggers for Sciatica Pain
Understanding and being mindful of triggers is a cornerstone in the healing journey from sciatic pain. Here are some triggers for flare ups:
- Poor Posture: Prolonged slouching or maintaining improper posture can strain the spine, potentially triggering sciatic pain.
- Heavy Lifting: Jobs or activities involving frequent heavy lifting put added stress on the spine, potentially intensifying sciatica. Employing proper lifting techniques is essential for prevention.
- Sedentary Habits: Extended periods of sitting, common in today's lifestyle, can contribute to sciatic pain. Taking breaks, incorporating stretches, and staying active can help alleviate discomfort.
Identifying and addressing these triggers empowers individuals in their journey to manage sciatic pain effectively. For personalized advice and targeted solutions, consulting with a healthcare professional is recommended.
7 Signs of Sciatica Improving
Witnessing signs of improvement in sciatica is a positive step in your journey to recovery. However, it's essential to recognize that improvement doesn't equate to complete healing. Proceed with caution to avoid triggering flare-ups, understanding that the healing process can manifest in various ways. The following signs provide valuable insights into the positive changes occurring, indicating that your efforts and treatments are making a difference. Let's explore these indicators of progress on the road to sciatic pain relief.
1.)Pain Reduction
One general, clear, and yes, obvious sign of sciatica improving is pain reduction. Experiencing a reduction in the intensity and frequency of sciatic pain is a reassuring and unmistakable sign that your efforts and treatments are positively impacting the healing process. This improvement is a visible indicator, but it's crucial to approach it with mindfulness.
Reduced pain doesn't necessarily signify the issue is fully resolved. Caution becomes paramount to avoid triggering flare-ups. While you navigate this phase of recovery, consider incorporating gentle exercises and stretches recommended by your healthcare professional to maintain flexibility.
One practical way to track this progress: keep a simple daily pain log rated on a scale of 1–10. Sciatica improvement is rarely a straight line, but a downward trend in both intensity and frequency of pain episodes over time is a reliable signal that healing is occurring.
2.) Pain Centralization
One of the most clinically significant and commonly overlooked signs that sciatica is improving is a concept called centralization. This occurs when pain that previously radiated all the way down your leg begins to retreat back toward the lower back and buttocks. Even if the pain in your lower back temporarily feels more intense, this movement toward the center of the body is a very positive indicator of nerve recovery.
Think of it this way: when sciatica first develops, pain typically travels downward from the lower back through the hip, buttock, and potentially all the way to the foot. As healing begins, that pain gradually reverses course and retreats upward toward its source. This is your nervous system beginning to decompress and heal.
It's equally important to recognize the opposite pattern, called peripheralization, when pain moves further down the leg toward the foot. Increased difficulty changing positions, or new pain when sneezing or coughing, are signs that things may be worsening rather than improving. If you notice peripheralization, contact your healthcare professional promptly.
Centralization can feel misleading at first. Your lower back pain may temporarily increase even as your leg symptoms improve. This is normal and represents progress, not regression. Always discuss these changes with your healthcare professional so they can confirm the pattern and adjust your treatment plan accordingly.
3.)Reduced Muscle Spasms
Similar to the notable relief experienced through pain reduction, a clear and reassuring signal of sciatica improving is the reduction of muscle spasms. A noticeable decrease in both the frequency and intensity of these spasms is very positive progress in your healing journey.
Just as with pain reduction, improvement doesn't mean the issue is fully resolved, emphasizing the importance of caution to prevent potential flare-ups. To sustain this relief, consider incorporating gentle exercises and stretches recommended by your healthcare professional. These practices aim to alleviate tension and support ongoing improvement. Additionally, prioritize aspects like hydration and nutrition, recognizing their impact on muscle health and their role in diminishing spasms.
4.)Increased Strength
Another notable sign of progress in sciatica recovery is the evident increase in strength. This positive development signifies that the muscles, previously weakened by sciatic pain, are beginning to become more responsive.
Observing this improvement involves noticing a substantial increase in muscle strength, especially in the areas directly affected by sciatic pain. The significance lies in the understanding that enhanced strength reflects a gradual recovery of the muscles from the impact of sciatica, promoting stability and resilience.
5.) Reduced Numbness & Tingling
As the sciatic nerve heals and inflammation around the nerve root decreases, one of the most meaningful signs of recovery is a reduction in numbness, tingling, or pins and needles sensations in the leg, foot, or toes. These sensations are a direct result of nerve compression, so as the nerve decompresses and begins to recover, normal sensation gradually returns.
It's worth noting that this improvement can sometimes feel like a temporary worsening before it gets better. As nerve fibers begin to reactivate, some patients notice increased tingling or heightened sensitivity before sensation fully normalizes. This is a recognized part of nerve healing, not a sign of regression.
If you find that your foot feels less numb, that sensation is returning to previously affected areas, or that the constant tingling is becoming less intrusive and less frequent, these are all very encouraging signs that the nerve is on the mend.
6.) Improved Sleep Quality
Sciatica can be relentless at night. The difficulty finding a comfortable position, combined with pain that often intensifies when lying still, makes restful sleep a significant challenge for many sufferers. That's why improved sleep quality is a meaningful and often underappreciated sign that your sciatica is improving.
As nerve inflammation reduces and pain intensity decreases, patients often report being able to find comfortable sleeping positions more easily, waking fewer times throughout the night due to pain, and feeling more rested overall. This improvement in sleep isn't just a comfort milestone. Quality sleep actively supports the body's tissue and nerve healing processes, creating a positive cycle that further accelerates recovery.
If sleep remains significantly disrupted despite other signs of improvement, speak with your healthcare professional. Persistent sleep deprivation can slow the healing process and may indicate that your treatment plan needs to be adjusted.
7.)Straight Leg Raise Test
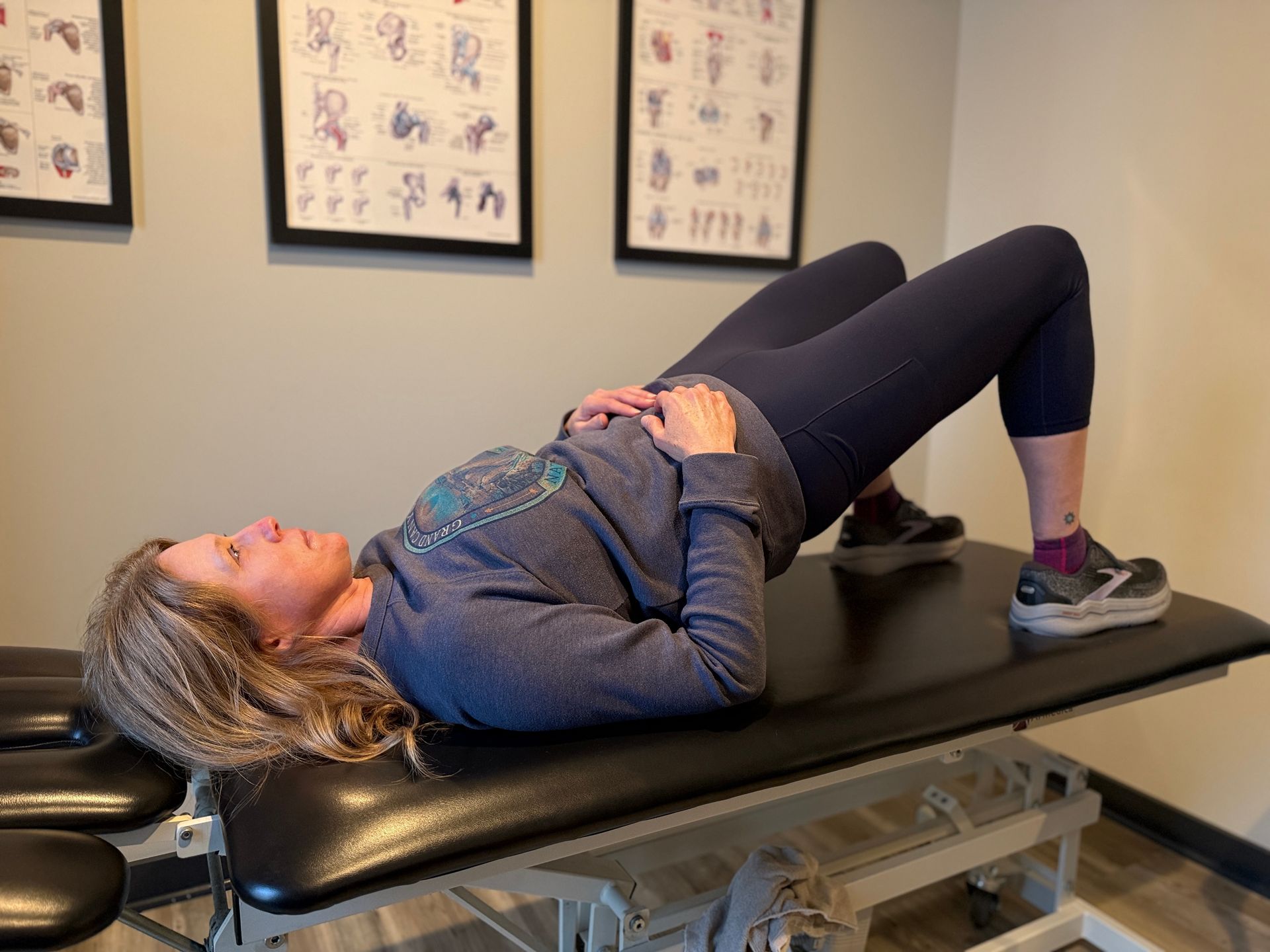
The straight leg raise test is a diagnostic evaluation commonly used to assess sciatic nerve involvement and monitor improvement in sciatica. To perform this test, lie on your back, and a healthcare professional will gently lift one of your legs, keeping it straight.
During the test, a healthcare professional gently lifts one leg while the patient lies on their back, noting the point at which discomfort or pain is felt. As recovery progresses, increased tolerance and reduced discomfort during the test become positive indicators of improvement. This test serves as a measurable and practical way for healthcare professionals to gauge the extent of sciatic involvement and monitor the effectiveness of treatments over time. Regular performance of the straight leg test provides valuable data, contributing to a comprehensive understanding of the individual's sciatic recovery process. Always consult with your healthcare professional for personalized insights tailored to your unique situation.
What to Expect: Sciatica Recovery Phases & Timeline
Recovery from sciatica is rarely a straight line, but it does tend to follow a recognizable pattern. Understanding these phases can help set realistic expectations and keep you motivated when progress feels slow.
Phase 1 - Acute Phase (Weeks 1 to 3):
This phase is focused on calming the nerve and managing initial inflammation. Pain is typically at its most intense during this period. Rest, gentle movement, and closely following your provider's guidance are the main priorities. Most patients begin to notice at least some reduction in acute pain within the first few weeks.
Phase 2 - Recovery Phase (Weeks 3 to 8):
As inflammation settles, this phase focuses on restoring mobility, reducing muscle tension, and beginning to rebuild strength. Centralization typically occurs during this phase, with pain retreating from the leg back toward the lower back. Targeted physical therapy exercises play a significant role here, and many patients begin to notice improvements in sleep and daily function.
Phase 3 - Rehabilitation Phase (Week 8 and beyond):
The final phase centers on returning to normal daily activities, rebuilding full strength and flexibility, and preventing recurrence. Most uncomplicated sciatica cases resolve within four to six weeks with consistent conservative care, though more severe cases may take longer. A personalized maintenance plan developed with your healthcare professional is key to staying well long-term.
What You Can Do to Keep Improving
As you journey through sciatic recovery, there are proactive steps you can take to foster continued improvement and enhance your overall well-being. Here are practical measures to integrate into your daily routine:
Consistent Exercise Routine:
- Engage in a tailored exercise program, emphasizing stretches and strengthening exercises recommended by your healthcare professional.
- Prioritize activities that promote flexibility, mobility, and overall muscle health.
Hydration and Nutrition:
- Stay adequately hydrated to support overall muscle health and recovery.
- Maintain a balanced diet rich in nutrients that contribute to the well-being of your muscles and nervous system.
Regular Breaks and Movement:
- If your daily routine involves prolonged periods of sitting, take regular breaks to stand, stretch, and move around. Additionally, you can spend time learning about office ergonomics to ensure a proper posture.
- Incorporate brief stretching sessions into your routine to prevent stiffness and promote circulation.
Stress Management:
- Explore stress-reducing practices, such as meditation, deep breathing exercises, or activities that bring relaxation.
- Stress management contributes to overall well-being and can positively impact your body's response to sciatic discomfort.
Follow Healthcare Guidance:
In your journey towards sciatic recovery, the guidance and expertise of healthcare professionals play a pivotal role. Adhering to the advice and recommendations provided by your healthcare professional is the compass that steers you through the path of healing. Regular attendance of scheduled appointments, proactive communication about any changes in symptoms, and active engagement in your personalized treatment plan will speed the process of your recovery.
Remember, your sciatic recovery is a collaborative effort, and your healthcare professional is there to guide and support you every step of the way. Whether it's monitoring progress through diagnostic tests like the straight leg raise test or implementing targeted exercises, their expertise forms a valuable resource on your path to recovery.
Frequently Asked Questions
How do I know if my sciatica is getting better or worse?
The clearest signs of improvement include decreasing pain intensity, centralization (pain retreating from the leg back toward the lower back), reduced numbness or tingling, improved sleep, and regaining strength and mobility. Signs that things may be worsening include peripheralization (pain traveling further down the leg toward the foot), increased difficulty changing positions, or new or worsening pain when sneezing or coughing. If you're experiencing these worsening signs, consult your healthcare professional promptly.
Can sciatica get worse before it gets better?
Yes, and this is one of the most important things to understand about sciatica recovery. Centralization, one of the primary signs of improvement, can temporarily increase lower back pain even as leg symptoms improve. Similarly, as nerves begin to heal and reactivate, some patients experience a brief increase in tingling before sensation fully normalizes. These experiences can feel like a step backward but are often actually signs that healing is occurring. Always consult with your healthcare provider if you're unsure whether changes in your symptoms represent improvement or worsening.
What does sciatica centralization feel like?
Centralization feels like a gradual withdrawal of pain from the lower leg and foot, back up toward the hip, buttock, and lower back. You may notice that your foot and calf feel less affected, while your lower back and buttock area may remain sore or feel slightly more intense for a period. This shift, even if the overall experience doesn't feel dramatically better at first, is a clinically positive sign. Over time, as centralization progresses fully, pain in the lower back should also decrease.
How long does sciatica typically take to heal?
Most cases of uncomplicated sciatica resolve within four to six weeks with consistent conservative care, including physical therapy, appropriate activity modification, and following your provider's guidance. More severe cases may take several months. Factors like age, overall health, activity level, and how early treatment was initiated all influence recovery time. Committing to a structured exercise and rehabilitation program is one of the most reliable ways to accelerate the process.
Should I exercise with sciatica, or will it make things worse?
In most cases, appropriate gentle movement is significantly better for sciatica recovery than complete rest. Staying active with exercises specifically recommended by your physical therapist or chiropractor helps reduce inflammation, maintain flexibility, rebuild strength, and prevent the muscle deconditioning that can prolong recovery. However, not all exercises are appropriate for every sciatica patient, and the wrong movements can aggravate symptoms. This is why a personalized exercise program developed with a healthcare professional is so important.
Connect with Us: